Past Research
Building on a Legacy of Innovation
Our past research in clinical neuropsychology has played a critical role in advancing patient care by improving our understanding of how brain function affects behaviour and cognition. We’ve pioneered the use of technology to track neurological health, enabling more accurate diagnostics and personalised treatments for conditions like neurodegenerative diseases and brain injuries. These innovations have not only enhanced the quality of care but have also empowered clinicians to monitor progress and adjust treatments in real time. Our achievements continue to guide future research as we push the boundaries of what’s possible in patient care and neurological health.
Get InvolvedExplore Current ResearchEvaluating Centralised Outcome Measurement
Explores the effectiveness of the FLX musculoskeletal (MSK) application in enhancing movement among individuals with brain injuries, who frequently experience co-morbid MSK disorders. Conducted over a 6-to-12-week period, the research utilised the Goal Manager® Outcome Measures Wizard (OMW) to track various metrics, including mood measures (GAD7, PHQ9), a customised International Classification of Functioning Disability and Health (ICF) Assessment, and weekly EuroQol 5 Dimension Scale (EQ5D) scores. Participants were recruited through social media and personal correspondence, and their technology confidence was assessed before and after the trial.
The results indicated significant improvements in MSK function due to the FLX interventions, underscoring the importance of centralised quantitative outcome tracking in rehabilitation. The study highlighted the practicality and efficiency of the OMW in clinical research, demonstrating its utility in managing diverse metrics. Overall, the FLX app proved to be an effective tool for enhancing musculoskeletal function in the brain injury population, providing valuable insights for future rehabilitation practices.
Want to Get Involved?
We'd love to hear from you! Contact us, to get involved in our exciting projects!
Get involved
Development of a Patient Portal application for paediatric rehabilitative care
The study highlights the often-overlooked perspectives of children and young people (CYP) in rehabilitation. The Goal Manager® application, initially designed for clinicians to organize and track rehabilitation data, was adapted to include a Patient Portal, co-designed with paediatric patients, their parents, and clinicians.
Funded by an Innovate Biomedical Catalyst Grant, the project involved virtual focus groups to gather insights from young people who had experienced brain injuries and undergone rehabilitation. The feedback informed the creation of wireframe designs and the refinement of key features, such as goal setting, expressing opinions on rehabilitation, and color-coding appointment details. The study emphasises the importance of accessibility and co-design in healthcare technology, ensuring that the Patient Portal meets the unique needs of CYP and supports their rehabilitation journey. This approach encourages meaningful, patient-led goal setting and could be applied to other healthcare technologies.

Developing a Data Dashboard for Quantitative Analysis of Rehabilitation Activity Data
Outline of the Data Dashboard project, funded through the Women in Innovation Award 2022/23. Shortlisted for the Poster Prize at UKABIF 2023, Manchester Presented at NR-SIG WFNR 2024, Coimbra Presented at Neuro Convention 2024, Birmingham

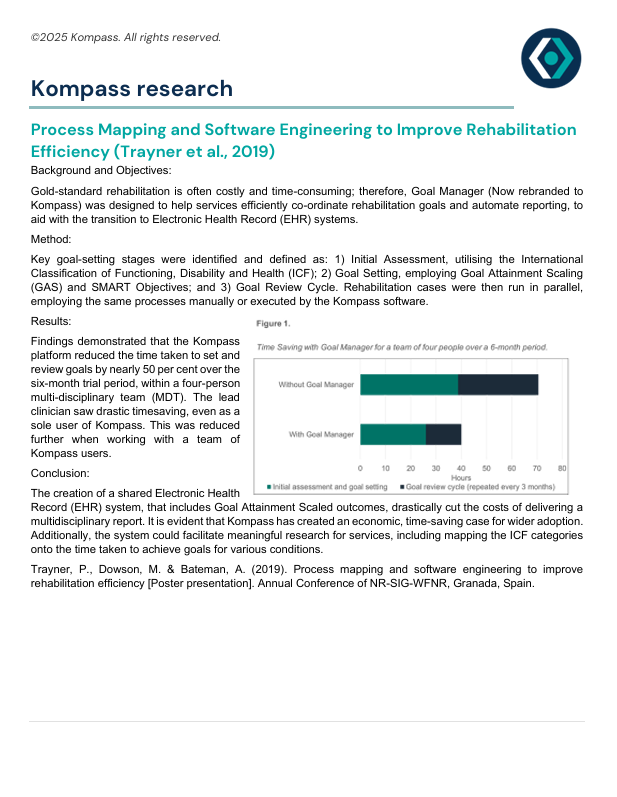
Process Mapping and Software Engineering to Improve Rehabilitation Efficiency
Examines the design and application of the Kompass platform in streamlining the rehabilitation goal-setting process and supporting the transition toward fully integrated Electronic Health Records (EHR). Presented at the NR-SIG-WFNR conference (Trayner et al., 2019), the study utilised process mapping methods to capture the full pathway of rehabilitation goal-setting—from initial assessment using the International Classification of Functioning, Disability and Health (ICF) to structured goal review through SMART objectives and Goal Attainment Scaling (GAS).
Embedding Co-Design in Digital Health: Responding to Gaps in Paediatric Neurorehabilitation
Kompass Kids was developed in collaboration with children, young people, and their families to bridge gaps in paediatric neurorehabilitation. Through co-design workshops and interviews, users shaped key features such as child-friendly goal setting, a patient passport for organising rehab information, and trusted resources to support continuity of care. By embedding lived experience at every stage, Kompass Kids delivers a practical, engaging, and empowering digital platform that supports recovery and helps young people take an active role in their rehabilitation journey.

Designed With, Not For: Embedding Young People’s Voices in Paediatric Rehabilitation
Paediatric rehabilitation too often relies on adult care models that don’t reflect the unique needs of children and young people. Through interviews with patients and families, we identified five key priorities for meaningful rehabilitation: personalised goals, fair access to care, clear progress tracking, reliable information, and empowerment. These insights directly shaped the development of Kompass Kids, a platform that supports goal setting, tracks progress, and provides trusted resources to give children and families more control over their rehabilitation journey. By embedding lived experience at every stage, Kompass Kids demonstrates how co-design can create more relevant, effective, and empowering care.



